By using this site, you are consenting to our use of cookies. To find out more visit our privacy policy.
The initial physical therapist visit consists of an examination and evaluation. Typically, these are completed in one visit, but they may occur over two or more visits.
Documentation elements for the initial examination and evaluation include the following: history (including review of systems), physical examination, tests and measures, diagnosis, prognosis, management plan, and plan of care.
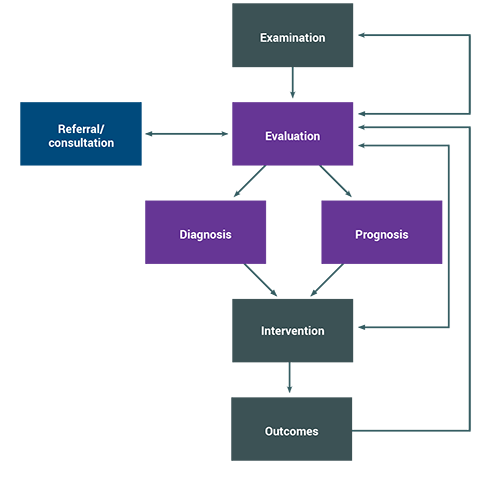
Guide to Physical Therapist Practice 4.0, Chapter 2
Patient and client management is an ongoing, iterative process that focuses on the evolving needs of each individual.
The physical therapist examination includes:
- History (including symptom investigation and review of systems).
- Physical examination.
- Tests and measures.
- Measuring outcomes.
Physical therapists conduct an examination to describe and/or quantify an individual's need for services. The PT is responsible for determining if there is sufficient information to:
- Conclude whether the individual would benefit from physical therapist services.
- Develop the management plan, including a plan of care if indicated.
- Progress the plan of care based on the individual's response to intervention.
Physical therapists also must determine whether referral to or consultation with another provider is indicated based on the information gathered during the initial encounter with the individual and during subsequent interactions.
The physical therapist must conduct an examination during the initial session with the individual prior to establishing a plan of care. The PT also collects data and information as part of each subsequent visit to determine any changes since the last visit, current status in specific areas, and whether the patient or client is progressing toward goals as expected. Tests and measures also are used to document the outcomes of the services provided.
Each component of the examination is described in further detail below:
History
The history is a systematic gathering of data — from both the past and the present — related to why the individual is seeking the services of the physical therapist. The data that are obtained include demographic information, social history, culture, employment and work history, growth and development, living environment, general health status, social and health habits (past and current), family history, medical and surgical history, current conditions or chief complaints, functional status and activity level, medications, and other clinical tests. While taking the history, the PT also identifies health restoration and prevention needs and coexisting health problems that may have implications for intervention.
The PT typically obtains this data from the individual, family, significant others, caregivers, and other interested parties (e.g., rehabilitation counselor, teacher, workers' compensation case manager, employer); through consultation with other members of the health care team; and through review of the individual's record. The image shows the types of data that may be generated from the history.

Guide to PT Practice, Chapter 3; Figure 3.1
Data from the history provides the initial information that the physical therapist uses to hypothesize about the existence and origin of impairments in body function and structure, activity limitations, and participation restrictions that are commonly related to medical conditions, sociodemographic factors, or personal characteristics.
For example, in the case of a 78-year-old woman who has a medical diagnosis of Parkinson disease and who lives alone, the medical diagnosis would suggest the possibility of the following impairments in body structure and function: loss of motor control, range-of-motion deficits, faulty posture, and decreased endurance for functional activities. Epidemiological research that is available about the activity limitations of older women, however, suggests that the performance of instrumental activities of daily living, or IADL, also may be problematic for that age group. In this case, then, the PT may use the information obtained during the history as well as the epidemiological information to create a hypothesis that would require further, in-depth examination during the tests and measures portion of the examination.
Pediatric Patients and Clients
The medical history may also include information about the mother's pregnancy and complications, the child's birth, neonatal complications, and age when the child achieved developmental milestones. In addition, the history includes information on the child's previous level of function and on the comorbidities that could affect the rate of recovery and rehabilitation. The social history may include information on the child's premorbid and current living environment, education, work status, and cultural preferences, including preferred language. The social history also includes information on the family: the child's parents, guardians, caregivers, siblings, and other important people in the child's life. Family history documents the resources, priorities, and needs of the family, including information on the child's daily routines, activities, and interests. Finally, the social history also includes information on child care, school, and other community activities, including play, leisure, recreation, and socialization.
The history of patients in a skilled nursing facility may be gathered from the hospital discharge summary, current and past facility assessments, previous minimum datasets, if applicable, and the nursing and consults section of the patient's medical record. Also, the physical therapist reviews documentation of the patient's previous restorative nursing program, if applicable, as this will alert the therapist to an understanding of the patient's prior level of function. It is critical for the PT, by reviewing records and interviewing patients and/or caregivers, to obtain an accurate social history and anticipated conclusion of care (discharge) disposition, including the current and potential support structure available to the patient upon discharge from the SNF. This information is needed for appropriate goal-setting and discharge planning in any setting, including long-term placement.
It is important for all providers to document a complete and thorough history that highlights pertinent information relevant to the patient's, client's, family's, or caregiver's reason for seeking physical therapist services. The history should clearly identify the patient, client, and family or caregiver concerns. The individual's medical and social history provides essential details used in the physical therapist's evaluation and determination of prognosis, goals, and the plan of care. For example, a patient or client with a wound who also has a history of diabetes may require increased intensity, frequency, and duration of services. Likewise, an individual with a history of a traumatic brain injury may have cognitive deficits or a loss of short-term memory that require an increased duration of services. Physical therapist management of a pediatric patient with cerebral palsy who is living in the foster care system may require coordination of services across multiple agencies and providers. The PT should clearly identify and explain the impact that these histories have on the current problem in the documentation of the evaluation and the plan of care.
Review of Systems
During the history-gathering phase, physical therapists also seek information about all major body systems to determine if the symptoms suggest the need for a referral for additional medical evaluation. This review of systems typically includes reports related to the following:
- Cardiovascular system.
- Pulmonary system.
- Endocrine system.
- Eyes, ears, nose, and throat.
- Gastrointestinal system.
- Genitourinary/reproductive systems.
- Hematologic and lymphatic systems.
- Immune system.
- Integumentary system.
- Nervous system.
- Musculoskeletal system.
The PT also documents reports related to the individual's overall physical (e.g., unexplained weight change, fatigue, lethargy, malaise) and emotional (e.g., anxiety, feelings of hopelessness) well-being.
Physical Examination
After organizing the available history information, the physical therapist begins the hands-on component of the examination. The physical examination begins with the systems review, which is a brief or limited examination of (1) the anatomical and physiological status of the cardiovascular and pulmonary, integumentary, musculoskeletal, and neuromuscular systems; (2) the communication ability, affect, cognition, language, and learning style of the individual; and (3) movement. The physical therapist especially notes how each of these last five components affects the individual's ability to initiate, sustain, and modify purposeful movement to perform an action, task, or activity that is pertinent to function.
The physical examination includes the following:
- For the cardiovascular and pulmonary systems: assessment of heart rate, respiratory rate, blood pressure, and edema.
- For the integumentary system: assessment of pliability (texture), presence of scar formation, skin color, and skin integrity.
- For the musculoskeletal system: assessment of gross symmetry, gross range of motion, gross strength, height, and weight.
- For the neuromuscular system: assessment of gross coordinated movement (balance, gait, locomotion, transfers, transitions) and motor function (motor control and motor learning).
- For communication ability, affect, cognition, language, and learning style: assessment of the individual's ability to make needs known, consciousness, orientation (person, place, time), expected emotional and behavioral responses, and learning preferences (learning barriers, education needs). The systems review for a pediatric patient also may include consideration of safety and well-being, nutrition, behavior and attention, and self-determination.
- Movement: the observation and assessment of movement and underlying impairments in the context of an individual’s function and performance.
Because individuals throughout the U.S. can now see a physical therapist without first getting a referral, an important reason for the PT to conduct the review of systems and physical examination, including the systems review within an examination, is that it may identify potential conditions that would require consultation with or referral to another provider. APTA's Code of Ethics for the Physical Therapist states: "Physical therapists shall make judgments within their scope of practice and level of expertise and shall communicate with, collaborate with, or refer to peers or other health care professionals when necessary."
For a number of reasons, such as an individual who has not seen a primary care provider recently, it may be the physical therapist who first recognizes a problem that requires further examination by another clinician. An experienced clinician can complete a review of systems in a relatively short time, but failure to do so can put patients or clients and the PT at risk.
Consider the following examples:
Case 1: A 38-year-old male with a complaint of knee pain presents to your clinic for an initial evaluation. As part of your initial examination and evaluation, you record his blood pressure at 160/98. After a discussion with the patient, you call his primary care physician regarding these findings, concerned that the patient may have undiagnosed hypertension. The patient returns a week later on a new medication to lower his blood pressure.
Case 2: A 47-year-old female with a recent left ankle sprain presents for an initial evaluation. In addition to weakness in her left ankle, you note weakness throughout her left side compared with the right side. This finding, along with others from the patient’s history and examination, may lead you to contact another provider in consideration of a more systemic cause of her symptoms.
Case 3: A 3-month-old infant who was born premature is referred to physical therapy with a diagnosis of torticollis. As part of your systems review, you note that the infant is unable to visually fix or track an adult face or a toy. You discuss a referral back to the child's pediatrician or an ophthalmologist.
Case 4: An 85-year-old male’s status of post-left hip replacement, with a prior level of function listed as independent, presents for an initial examination. During the systems review, the patient presents with moderately impaired cognition that varies significantly from the current and prior level of function that is documented in the nursing portion of the assessment. The PT alerts the nurse and refers the patient to his primary care physician for reassessment before starting treatment.
Case 5: A 72-year-old female with a past medical history of hypertension, anemia, GI bleeds, wrist fractures, and degenerative joint disease is referred for gait training, pain management, and strengthening after a thoracic compression fracture. During the chart review, the PT notes that the patient has been prescribed an anti-hypertensive medication, a selective estrogen receptor modulator, and a nonsteroidal anti-inflammatory. After the patient interview and initial review of the systems, the PT asks to see the patient's medications. The patient reports the previously known medications but also states that she is taking a daily antidepressant and aspirin. Because of the patient's history of GI bleeding and anemia, the PT questions her regimen of aspirin and NSAID and calls her primary physician to ensure that he is aware the patient is taking both. It turns out he is not aware, and he gives the PT a verbal order to discontinue the aspirin. The PT advises the patient of the verbal order, documents the discussion, the order, and the consultation with the physician, and communicates the exchange to a nurse manager.
Tests and Measures
Tests and measures are yet another means of gathering data about the individual. Physical therapists use tests and measures during the initial examination to rule in or rule out causes of impairment in body structures and functions, activity limitations, and participation restrictions. From the information gathered in the history and systems review, the PT determines a hypothesis for a diagnosis or diagnoses. The PT then determines which tests and measures are required to further prove (or disprove) the hypothesis.
The physical therapist performs only the tests and measures necessary to (1) confirm or reject a hypothesis about the factors that contribute to making the individual's current level of function less than optimal and (2) support the PT's clinical judgments about the diagnosis, prognosis, management plan, and plan of care.
Before, during, and after administering the tests and measures, the physical therapist gauges the patient's responses, assesses physical status, and obtains a more specific understanding of the condition and the diagnostic and therapeutic requirements of managing that condition.
The physical therapist may decide to use one, two, or more, or portions of several specific tests and measures as part of the examination, based on the purpose of the visit, the complexity of the condition, and the directions taken in the clinical decision-making process.
The physical therapists may conduct an examination that includes a selection of appropriate tests and measures after the history, review of systems, and systems review. On the other hand, the PT may conclude from the history and systems review that further examination and intervention are not required, or that the individual should be referred to another practitioner, or both. Even within a full examination, the PT may uncover additional problems as the examination progresses and may conduct additional tests and measures to obtain sufficient data to perform an evaluation, establish a diagnosis and a prognosis, and determine the plan of care. What this means is that the length of an examination can vary widely, as necessary.
The tests and measures selected by the physical therapist should yield data that is sufficiently accurate and precise to allow the PT to make a correct inference about the individual's condition. The selection of specific tests and measures and the depth of the examination vary based on the age of the individual, the severity of the problem, the stage of recovery (acute, subacute, or chronic), the phase of rehabilitation (early, intermediate, late, return to activity), the individual's home, community, or work situation, and other relevant factors.
Tests and measures vary in their precision, but even those that are less precise can yield useful data. For instance, data generated from either a gross muscle test of a group of muscles or a very precise manual muscle test could be used to reject the hypothesis that muscle performance is contributing to an activity limitation. Similarly, even though a functional assessment instrument may quantify ability in a large number of ADLs or IADLs, it may fail to detect the individual's inability to perform a particular task or activity that is most important to that person. There is no specific recommendation for how tests and measures are ordered or displayed; however, the PT should make the record of findings easy to follow. The PT may choose to document certain systems together, follow a natural progression of an evaluation by patient position (e.g., from seated to supine to prone to standing), or have the patient complete simple tasks before complex activities. In pediatrics, the PT may decide to present the tests and measures related to participation and activity (function) before the tests and measures related to body structure and function.
In addition to more traditional tests and measures (e.g., ROM, strength, balance, edema), the physical therapist should rely on standardized tests and measures. These standardized tests can be specific to a diagnosis, such as knee and low back, or a more general measure relating to disability. The test and measure may be performance-based or may be patient-reported.
Choosing standardized tests and measures requires careful thought and consideration, including factors such as the individual's tolerance of testing, the time involved, the environment, and the psychometrics of the test. Some tests will quantify pain or function, while others measure the degree of impairment or disability. In addition, some tests are diagnostic, while others are more prognostic in their intent. Appropriate use of standardized tests and measures is valuable in determining the patient's or client's progress and outcomes throughout the episode of care and can provide a standard measure of comparison for clinical outcomes.
Also critical is the use of a measure that is relevant to each individual or to the population being measured. The stronger the psychometric properties and the closer the match of the study group for the outcome tool with the individual or population that the physical therapist is measuring, the more accurate and useful that measurement will be.
Pediatric Patients and Clients
In pediatric practice, outcomes are often documented by the achievement of behavioral objectives; thus, the documentation of initial tests and measures should be precise to record the pediatric patient's current status on identified priority tasks, including the conditions and criteria under which the behaviors are demonstrated. Tests and measures at the participation level should be conducted in the pediatric patient's or client's natural environments when appropriate — at home, school, or in the community. Observations made during key routines and activities, such as negotiating from the bus to the classroom or negotiating playground equipment, should be documented.
Tests and measure summaries with psychometrics and clinical insights can be found on APTA's Evidence-Based Resources webpage.
Selecting Outcome Tools
The physical therapist selects the appropriate standardized outcome measures to quantify the individual's status just prior to, during, and at the conclusion of an episode of care. The therapist might choose self-report or performance-based tools or general or specific measures. The use of standardized outcome measures that have sound psychometric properties is critical in determining the outcome status of an individual or population.
Also critical is the use of a measure that is relevant to each individual or to the population being measured. The stronger the psychometric properties, and the closer the match of the study group for the outcome tool with the individual or population that the physical therapist is measuring, the more accurate and useful that measurement will be.
Establishing a Baseline and Outcome Status
The use of standardized tests and measures early in the episode of care establishes the baseline status of the individual, providing a means to quantify change in functioning. Beginning with the history, the physical therapist identifies the individual's expectations, perceived need for physical therapist services, personal goals, and desired outcome status. The physical therapist then considers whether the desired goals and outcome status are realistic in the context of the examination data and the resulting evaluation, which includes determining the diagnosis. Based on this information and the underlying pathology or health condition causing the impairments of body functions and structures, activity limitations, and participation restrictions, the physical therapist then generates a prognosis intended to predict likely outcomes.
Evaluation
Evaluation is the process by which the physical therapist:
- Interprets the individual's response to tests and measures.
- Integrates the test and measure data with other information collected during the history and systems review.
- Determines a diagnosis or diagnoses amenable to physical therapist management.
- Determines a prognosis, including goals for physical therapist management.
- Develops a management plan and plan of care.
There are three CPT codes used for determining the complexity of a physical therapy evaluation. Specific to choosing the CPT evaluation code that best reflects the correct level of complexity are four components that must be included in the documentation.
The four primary components and the process to use to inform the selection of the evaluation complexity level are:
- History (medical and functional) and impact of "contextual factors."
- Examination (includes body structures and functions, activity limitations and/or participation restrictions, environmental, and personal factors).
- Leads to the ability to describe clinical presentations.
- Leads to the ability to make clinical judgments to develop a plan for managing the patient through an episode of care.
The code selected will tell payers the complexity level of an evaluation based on your patient's clinical presentation and your clinical decision-making. In doing so, you must provide documentation supporting your choice. The chart below will guide you in providing the appropriate documentation. Keep in mind that to support your code selection, you must clearly document each required component for that code. If even one component cannot be supported, you must report a lower level of complexity. There is no mandated format for the required documentation, but you should make the components readily apparent to all third parties reading and reviewing your report of the patient's evaluation.
|
Required Component |
Supporting Documentation |
|
Personal Factors, Comorbidities |
|
|
Body Systems Elements (Body Structures and Functions, Activity Limitations, Participation Restrictions) |
|
|
Clinical Presentation |
|
|
Clinical Decision Making |
|
|
Functional Outcomes Tools |
|
|
Evaluation Complexity Level |
|
The evaluation reflects the chronicity or severity of the current problem, the possibility of multisite or multisystem involvement, the presence of preexisting systemic conditions or diseases, and the stability of the condition. Physical therapists also consider the severity and complexity of the current impairments and the probability of prolonged impairment of body structures and functions; activity limitations and participation restrictions; the living environment; potential destinations at the conclusion of the episode of care; and social support.
Evaluation occurs at the start of care and continues throughout the episode of care to determine the individual's response to interventions and progress toward identified goals.
An evaluation is a thought process that may or may not include formal documentation. This evaluative process is a synthesis of all of the data and findings gathered from the examination and collaborative decision-making with the patient or client. The evaluation process leads to documentation of such items as impairments, activity limitations, and participation restrictions. It should guide the physical therapist to a diagnosis and prognosis for each patient or client.
Pediatric Patients and Clients
Consistent with family-centered care, the documentation of the evaluation reflects a strength-based approach. An evaluation would typically include the pediatric patient's strengths, readiness to learn a new skill, and areas of concern, priority, or need. Areas of need would include the patient's participation restrictions in the home, school, and community; activity limitations; and body structure and function impairments. The evaluation should also note characteristics of both the patient and their environment hypothesized to be facilitators or barriers to their activity and participation.
The documentation of an evaluation can use formats such as a problem list or a statement of assessment with key factors (e.g., cognitive factors, comorbidities, social support) influencing the patient or client status. While the documentation of an evaluation may come in different formats, the record should convey to the reader what examination factors are relevant to the current complaint. The evaluation process should arrive at a physical therapist diagnosis and a prognosis for a functional outcome(s) at the conclusion of physical therapist services.
Consider the following examples:
Narrative
Clinical impression: Patient is a 68-year-old female with significant limitations in right knee AROM, strength, weight-bearing tolerance. Patient is also limited due to pain and edema in the right leg. Patient requires assistance for transfers, bathing, dressing, grooming, and gait at this time. Patient was independent in all activities prior to admission, is otherwise in good health, and has good family support. Patient requires physical therapist intervention to resume normal activity.
Pediatric Patients and Clients
Narrative
Patient is a 3-year-old boy with significant developmental delays. He is able to communicate to show his likes and dislikes, walks independently, feeds himself finger foods, and manipulates toys with both hands. He can attend to structured learning activities and remember routines and activities. He has a very supportive family and two playful siblings. He is ready to learn to use his motor abilities during play activities and games with other children. Currently, the child does not spontaneously initiate play with peers or siblings and has limited verbal communication. He has difficulty with jumping and ball skills. He requires supervision on stairs, assistance for eating with utensils, dressing, and bathing, and he occasionally falls on outdoor terrain. He requires physical therapist intervention to promote his strength, balance, and motor planning, especially considering weakness on his left side. A consistent team approach for communication and positive behavior support is recommended.
Problem list:
- Impairments: Edema, impaired balance, impaired gait, impaired joint mobility, impaired muscle strength, and pain.
- Activity limitation: Inability to stand without minimal assistance, inability to ambulate greater than 20 feet with moderate assistance, requires setup for bathing, and minimal assistance for dressing.
- Participation restrictions: No spontaneous play with siblings and peers.
- Environmental factors: Environmental barriers and home barriers present.
Diagnosis
Diagnostic labels may be used to describe multiple dimensions of the individual, ranging from the most basic cellular level to the highest level of functioning as a person in society. Making a diagnosis requires the clinician to collect and sort data into categories according to a classification scheme relevant to the clinician who is making the diagnosis.
These classification schemes should meet the following criteria:
- The classification schemes must be consistent with the boundaries placed on the profession by law (which may regulate the application of certain types of diagnostic categories) and by society (which grants approval for managing specific types of problems and conditions).
- The tests and measures necessary for confirming the diagnosis must be within the legal purview of the health care professional.
- The label used to categorize a condition should describe the problem in a way that directs treatment options that are within the legal purview of the health care professional who is making the diagnosis.
Although physicians typically use labels that identify disease, disorder, or condition at the level of the cell, tissue, organ, or system, physical therapists use labels that identify the impact of a condition on function at the level of the system and the integration of all systems to produce movement.
Physical therapists use a systematic process to classify an individual into a diagnostic category. This process includes integrating and evaluating the data from the examination to describe the individual's condition in terms that will guide the PT in determining the prognosis and developing a management plan and plan of care. Thus, the diagnostic label indicates the primary dysfunctions toward which the PT directs intervention. The diagnostic process enables the PT to verify the needs of each individual relative to similar people who are classified in the same category, while also capturing each individual's unique concerns within a particular sociocultural and physical environment.
The physical therapist uses the diagnostic process to identify discrepancies between the individual's desired level of function and their capacity to achieve that level. In carrying out the diagnostic process, the PT may need to obtain additional information (including diagnostic labels) from other professionals. As the diagnostic process continues, the PT also may identify findings that should be shared with other professionals (including referral sources) to ensure optimal care. If the diagnostic process reveals findings that are outside the scope of the PT's knowledge, experience, or expertise, the PT refers the individual to an appropriate, qualified provider.
Even if the diagnostic process does not yield an identifiable cluster (of signs or symptoms, impairments in body structures and functions, activity limitations, or participation restrictions), syndrome, or category, the physical therapist may administer intervention for the alleviation of symptoms and remediation of impairments. As in all other cases, the PT is guided by individual responses to intervention and may determine that a reexamination is in order and proceed accordingly.
The International Classification of Functioning, Disability and Health was developed by the World Health Organization in 2001 and endorsed by APTA in 2008. The ICF, with a focus on human functioning, provides a unified, standard language and framework that facilitates the description of the components of functioning that are impacted by a health condition. It enables data collection on how people with a health condition function in their daily lives rather than on their diagnosis or the presence or absence of disease. The ICF describes the situation of the individual within health and health-related domains and within the context of environmental and personal factors.
A diagnosis is determined by the physical therapist after the examination and evaluation process and typically is made at the impairment, activity, and participation levels.
The diagnosis by a physical therapist should be clearly documented and can take different formats. Physical therapists may select the corresponding ICD-10 code or ICF classification that reflects the results of the examination and evaluation process.
For billing purposes, diagnoses are coded according to ICD-10. When coding diagnoses by ICD-10 for reporting purposes, you may be required to use codes that relate to the impairment for which you are treating the patient or client. In fact, some payers have specific policies for reporting medical and treatment diagnoses, such as Medicare's Local Coverage Determinations, so it is important to be familiar with the specific payer policies. Some payers prefer as much specificity in ICD-10 coding as possible. Therefore, it is recommended that you have a current ICD-10 book. APTA's ICD-10-CD webpage has additional information on ICD-10 coding.
In April 2017, the APTA Board of Directors adopted the Movement System Diagnosis criteria to be used by any interested parties developing diagnostic systems and labels.
Pediatric Patients and Clients
To meet the requirements of various pediatric practice settings, medical diagnoses may also be noted. For example, in early intervention, physical therapy diagnosis is included secondary to medical diagnosis as being one criterion for eligibility of services under the Individuals with Disabilities Education Improvement Act. In school-based practice, one of the disability categories under IDEA is similarly reported to document the eligibility of services. In both early-intervention and school-based practice, the multidisciplinary individualized family service plans, or IFSPs, and individualized education programs, or IEPs, include only a medical diagnosis; a physical therapy diagnosis is not included.
Note 1: Certain state practice acts contain specific regulations regarding a physical therapy diagnosis. Review the FSBPT regulatory resources for information about your state practice act.
Note 2: Third-party payers also may specifically identify ICD-10 codes paired with CPT codes that are considered to be medically necessary.
Prognosis
Once the diagnosis has been established, the physical therapist determines the prognosis. The prognosis is the determination of the predicted optimal level of improvement in function and the amount of time needed to reach that level. It also may include a prediction of levels of improvement that may be reached at various intervals during the course of physical therapy.
In determining the prognosis, PTs must consider the differences between the highest level of function of which the individual is capable and the highest level of function that is likely to be habitual for that individual. Individuals are more likely to achieve the goals and outcomes that are determined with the physical therapist if they perceive a need to function at the highest level of their ability and if they are motivated to function habitually at that level. Thus, understanding the difference between what a person currently does and what that person potentially could do is essential in making a prognosis and identifying realistic, achievable goals and outcomes. Physical therapists ultimately must abide by the decisions of the individual regarding actions, tasks, and activities that will be incorporated into a daily routine and regarding what constitutes a meaningful level of function.
Documentation of the prognosis conveys the physical therapist's professional judgment for the individual's predicted functional outcome and the required duration of services to obtain this functional outcome. It is important to differentiate between the individual's medical prognosis and their rehabilitation prognosis. The PT also should consider the prognosis for the entire episode of care and not just one specific time frame, such as the acute care stay, as this may significantly affect options for continued physical therapy and/or other forms of skilled care.
Pediatric Patients and Clients
In pediatrics, it is recommended that therapists document the clinical reasoning that supports the stated prognosis. For example: "The child's prognosis for independent walking is positive secondary to the child presenting with a Gross Motor Functional Classification System level of I and a supportive family who provide appropriate movement opportunities."
Management Plan and Plan of Care
The management plan is based on the best available evidence and may include recommendations and goals developed by other entities. When indicated, the management plan describes the need for additional testing or other information to inform decision-making regarding the need for ongoing physical therapist services. A management plan is established in collaboration with the individual and, when appropriate, others involved in their management. The management plan includes interventions that address impairments, improve or restore movement patterns, and facilitate a return to the specific activities a person performs for life participation. Delegation and supervision of interventions as appropriate are included in the management plan. The management plan can describe an episode of care or services such as prevention, health promotion, or wellness services in groups or populations. Physical therapists foster and encourage lifelong and long-term patient and client relationships. Where feasible, physical therapists, as entry-point providers, provide services within the community that are available to individuals over a lifetime. Efforts are made to address movement disorders and to maintain optimal health and wellness through physical therapist intervention as needed.
The plan of care consists of statements that specify the goals, predicted level of optimal improvement, specific interventions to be used, and proposed duration and frequency of the interventions that are required to reach the goals and outcomes.
The physical therapist establishes the plan of care in collaboration with the individual and, when appropriate, others involved in the individual's care. The plan is based on the data gathered from the examination (history, systems review, and tests and measures) and on the diagnosis and prognosis determined by the physical therapist. In designing the plan of care, the PT analyzes and integrates the clinical implications of the severity, complexity, and acuity of the pathology and pathophysiology (disease, disorder, or condition), the impairments in body functions and structures, the activity limitations, and the participation restrictions to establish the prognosis.
The plan of care identifies the individual's goals, which are the intended impact on functioning (body functions and structures, activities, and participation) as a result of implementing the plan. Goals should be measurable, functionally driven, and time-limited. If required, the goals may be classified as short-term and long-term. The plan of care includes plans anticipated at the conclusion of the episode of care. In consultation with appropriate individuals, the physical therapist plans for the conclusion of care and provides for an appropriate follow-up or referral. The primary criterion for the conclusion of care is the achievement of the individual's goals. When the episode of care is concluded prior to the achievement of identified goals, the individual's status and the rationale for the conclusion of care are documented. For individuals who require multiple episodes of care, periodic follow-up is needed over the lifespan to ensure safety and effective adaptation following changes in physical status, caregivers, environment, or task demands.
Documentation of the plan of care includes the following components, all of which are further described below:
- Overall goals are stated in functional, measurable terms that indicate the predicted level of improvement in function. These goals are made in collaboration with the patient or client and other appropriate stakeholders.
- A statement of interventions and treatments to be provided during the episode of care.
- Duration and frequency of service are required to reach the goals.
- Anticipated plans for the conclusion of care may be part of the prognosis or written separately.
- For pediatric patients and clients:
The plan of care for a pediatric patient from birth to age 3 can be embedded in the IFSP. The plan of care for a patient of school age (3-21) can be embedded in the IEP or documented in a 504 plan as a supplemental service to support modifications and adaptations within the school environment. In both early intervention and school-based services, the IFSP and IEP are developed through team collaboration that includes the family and, when appropriate, the pediatric patient. In early intervention, the plan of care includes preparations for the patient to transition out of early intervention. In school-based services, the plan includes transitioning the student to adulthood at age 16.
*Note: Medicare includes diagnoses within its documentation requirements for the plan of care. See the Medicare Benefit Policy Manual, Section 220.1.2.B.
Physical therapists develop goals with the patient or client and, when appropriate, family or caregiver at the onset of care for a variety of reasons. Goals provide an opportunity for the individual and/or family or caregiver to describe what functional changes they hope to accomplish through physical therapist services. The goals established during an initial evaluation and determination of the patient's or client's prognosis provide the foundation on which the plan of care is directed. However, the goals are dynamic, and PTs demonstrate progression (or lack of progression) and ongoing communication of expected outcomes and conclusion of care (discharge) planning through updates, changes, deletions, and additions to these initial goals in subsequent documentation (daily notes, summaries, and reexaminations).
Goals can be written to address impairments, activity limitations, participation restrictions, and prevention. To use goals effectively to direct the progression of physical therapist services, PTs should make them objective and measurable by reevaluation, related to the individual's impairment, activity limitation, and participation restriction, and include anticipated time frames. In addition, PTs should document goals in functional terms related to the individual rather than to the PT. Writing goals in functional terms is important because it shows how the goals support both the medical necessity of the physical therapist services and the need for the skilled intervention of the PT or physical therapist assistant. Functional goals are a PT's means of conveying to external stakeholders why this individual requires physical therapist services; they are not simply a checklist of what needs to be accomplished. Consider the following examples:
- Increase shoulder flexion to 150 degrees.
- Decrease pain.
- Improve safety.
The above goals do not identify the specific needs of a patient or client. It is important to express why the individual needs to increase their ROM or level of assistance. Nor do the above goals include measurable metrics such as time frame, distance, and level of assistance. Here are more functional characterizations of the above goals:
- The patient will increase shoulder flexion to 150 degrees to enable overhead activities within one week.
- The patient will decrease pain level to 2/5 on VAS with reaching activities within two weeks.
- The patient will increase mobility to enable her to safely walk with a standard walker independently within the home to complete activities of daily living upon discharge from the SNF.
Medicare and third-party payers determine the physical therapy benefit or continuation of physical therapist services based on the provision of skilled services to provide care that is reasonable and necessary to prevent or slow further deterioration. In other words, payers want to see evidence of skilled therapy services. Coverage cannot be denied based on the absence of potential for improvement or restoration, and so in certain circumstances, therapists may need to communicate very clearly what this means for the patient or client. For example, for some individuals, progressing from a maximum level of assistance to a moderate level of assistance may not show a significant change in status. However, if that degree of change represents the individual's ability to go home with caregiver support, this must be conveyed in the documentation.
The physical therapist determines time frames for the achievement of goals and outcomes to maximize the effectiveness of care while remaining realistic. Goals may be written in terms of time (i.e., days, weeks, or months) or in terms of visits in which the goal will be achieved. PTs also can clarify if the goal is short term or long term. A short-term goal implies that the patient or client will achieve the activity in the near future (e.g., in a day or within a week) or may indicate a change that needs to occur before long-term or outcome goals can be met or exceeded by the patient or client.
Finally, goals should be designed based on collaboration with the patient, client, and/or family or caregiver. The documentation should reflect both collaboration and agreement on the goals. Updating goals during a physical therapy episode of care is important to clinical practice and should be documented clearly and frequently. Documentation of goals after the initial evaluation will be discussed in later sections.
Components of well-written goals include:
- Identification of the individual who is receiving therapy and will carry out the program. This is generally the patient or client, but it may also be the caregiver or family members.
- Description of the movement or activity that the individual will perform, such as a stand-pivot transfer from bed to chair.
- A connection of the movement or activity to a specific function, such as to eat breakfast or to perform dressing.
- Specific conditions in which the movement or activity will be performed, such as with full weight bearing on both lower extremities or with the use of a walker.
- Factors for measuring performance, such as with contact guard assistance or with 2/5 pain on VAS.
- The time frame for achieving the goal.
Examples:
- Short-term goal: Within one week, patient will safely walk from his bedroom to the bathroom with a walker in two minutes to prevent accidents that may lead to falls.
- Short-term goal: Within two visits, patient will report a decrease in pain in the right shoulder after exercise to 2/10 to enable her to move with her walker in her home.
- Short-term goal: Within three visits, patient will demonstrate ambulation with a standard walker x 100 feet with contact guard and stable vital signs.
- Short-term goal: Patient will perform stand-pivot transfers from bed to chair with full weight bearing on both lower extremities and contact guard assistance within one week in order to decrease risk of falls with transfers.
- Long-term goal: Within three weeks, patient will ambulate independently with a straight cane greater than 500 feet for community activities.
- Long-term goal: Patient will walk 200 feet independently on level surfaces with a straight cane, so he can attend the dining room for three meals a day within one month.
- Pediatric long-term goal: Within six months, the pediatric patient will walk with one hand held from the family room to the kitchen, a distance of 25 feet, at dinner time.
- Pediatric long-term goal: Pediatric patient will sit independently on the floor with both hands free to play with a toy within six months.
After the initial evaluation, updating the goals shows others how the patient or client is achieving (or not achieving) the predicted outcome. If an individual achieves a goal, this should be documented so others may also know what the patient or client has achieved. This is important in all settings so other health care providers (i.e., nurses, physicians, case managers, etc.) will know that the patient or client has achieved the goal. These changes will then drive the subsequent care of the patient and client. Clearly documenting updates of a patient's or client's physical therapy goals communicates to third-party payers any functional changes in a patient's or client's status and the benefits of the service, along with the need for continued services, if indicated.
The goals should be updated regularly, depending on the length of the episode of care. The goals also should be updated whenever there is a change in the patient's or client's progress or medical status. When goals are initially set by the physical therapist in conjunction with the patient or client and/or family or other caregivers, the achievement of the goals is dependent on many factors that may affect the individual's progress toward the goals. The PT makes the best prediction of when a patient or client will accomplish the goals, but this can change for a variety of reasons. For example, if the goal is to transfer from bed to chair with minimal verbal cues within three days but the individual has more difficulty with bed mobility than expected (an essential component of the goal achievement), then the goal would need to be revised in terms of time frame or level of assistance.
Note: State laws and certain third-party payers may have specific expectations on how often goals are updated.
What if an individual does not demonstrate the expected progress toward their goals? In this case, the PT must analyze and consider any factors that may have prevented progression. Was there a medical issue that prevented progression? Was the individual unable to participate in physical therapy interventions as expected? Whenever there is little or no progress toward the anticipated goals, the reasons for the delay should be clearly documented and discussed. The PT also should indicate what measures are being taken to overcome the problems over the next treatment period. Documentation of these clinical decision-making processes indicates the physical therapist's involvement in the overall care management of the patient or client.
Keep in mind that goals do not always involve "improvement" in the patient's or client's condition. The Jimmo v. Sebelius settlement clarified that skilled services to maintain or manage a patient's current condition when no functional improvement is possible are covered under Medicare. It is essential, however, to document accurately the skilled maintenance services to safeguard against unfair denials by Medicare contractors for skilled therapy services that aid in maintaining a patient's current condition or to prevent or slow decline. APTA's Skilled Maintenance webpage provides details on documentation specific to maintenance goals as opposed to restorative goals.
Interventions for the Plan of Care
Physical therapists purposefully interact with the individual and, when appropriate, with other people involved in the individual's care, using various interventions to produce changes in the condition that are consistent with the diagnosis and prognosis.
Generally, there are five overall intervention strategies:
- Remediation.
- Adaptation.
- Compensation.
- Task modification.
- Environmental modification.
Categories of physical therapist interventions include education and procedural interventions.
The process of informing, educating, or training individuals, families, significant others, and caregivers is intended to promote and optimize physical therapist services. Instruction may be related to the current condition; specific impairments in body structure or function, activity limitations, or participation restrictions; a plan of care; a need for enhanced performance; a transition to a different role or setting; risk factors for developing a problem or dysfunction; or a need for health, wellness, or fitness programs. PTs are responsible for individual instruction across all settings for all individuals.
Procedural interventions describe the services provided by the physical therapist and physical therapist assistant under the direction and supervision of the physical therapist. The following are descriptors of procedural interventions:
- Adaptive and assistive technology.
- Biophysical agents.
- Functional training in self-care and domestic, work, community, social, and civic life.
- Integumentary repair and protection techniques.
- Manual therapy.
- Motor function/movement training control.
- Respiratory and ventilatory techniques for enhanced respiratory function.
- Therapeutic exercise.
The physical therapist selects, prescribes, and implements interventions based on examination data, the evaluation, the diagnosis and prognosis, and the goals for a particular individual. Depending on the individual's response to intervention, the PT may decide that reexamination is necessary, a decision that may lead to different therapeutic methods or techniques or, alternatively, the conclusion of the episode of care.
Decisions about the type and intensity of other interventions are based on the PT's assessment of the individual's current condition and are contingent on the timely monitoring of the individual's response and the progress made toward achieving the goals. In prescribing interventions for an individual, the PT includes parameters for each intervention, such as method, mode, or device; intensity, load, or tempo; duration and frequency; and progression.
Factors that influence the complexity, frequency, and duration of the intervention and the decision-making process may include:
- Accessibility and availability of resources.
- Adherence to the intervention program.
- Age.
- Anatomical and physiological changes related to growth and development.
- Caregiver consistency or expertise.
- Chronicity or severity of the current condition.
- Cognitive status.
- Comorbidities, complications, or secondary impairments.
- Concurrent medical, surgical, and therapeutic interventions.
- Decline in functional independence.
- Level of impairment.
- Level of physical function.
- Living environment.
- Multisite or multisystem involvement.
- Nutritional status.
- Overall health status.
- Potential destinations at the conclusion of the episode of care.
- Premorbid conditions.
- Probability of prolonged impairment in body structures and functions, activity limitations, or participation restrictions.
- Psychosocial and socioeconomic factors.
- Psychomotor abilities.
- Social support.
- Stability of the condition.
It is important that physical therapists consider a number of factors when they write the plan of care for each individual. Factors to consider include, but are not limited to, the following:
- The patient's or client's status, including physical, cognitive, and emotional factors (e.g., acuity, prognosis, learning barriers, language barriers, cultural differences).
- The patient's or client's expected progression.
- Planning for disposition of the conclusion of the episode of care (see below).
- Whether or not additional staff, either another PT or a PTA, will provide some of the interventions during the episode of care.
- The physical therapist plan of care in a skilled nursing facility is incorporated into the patient's individualized, interdisciplinary comprehensive care plan, which reflects problem areas documented through data obtained on the minimum datasets. The PT should initiate and document patient and caregiver training in addition to providing the results of the initial evaluation to the interdisciplinary team.
Pediatric Patients and Clients
The physical therapist plan of care in early intervention and school-based practice is often incorporated into the pediatric patient's general team intervention plan provided in the IFSP or IEP, respectively. The general plan may also include general methods or strategies that the team will use to assist the patient and family in early intervention or the student in school-based practice in meeting their goals. More specific details regarding the intervention strategies are contained in the PT's supplemental intervention plan or daily visit documentation notes.
When a physical therapist is providing care in conjunction with a physical therapist assistant, the documented plan of care should be a clear communication tool for the coordination of care. It is this documented plan of care, along with verbal communications as indicated, that guides the PTA in following the PT's plan during the episode of care.
Consider the following examples:
- Gait training, therapeutic exercises, modalities.
- Gait training with standard walker — progress distance up to 100 feet with stable vital signs.
- Therapeutic exercises for both lower extremities — avoid flexion past 90 degrees; add up to five pounds of weight once AROM is within 15 degrees of normal limits.
- Pulsed ultrasound to bilateral knees 1.5 W/cm2 X 5 min per knee after therapeutic exercise.
Example 2: Providing more information is a much better tool for communicating with other staff. Writing a more detailed plan of care can improve patient or client safety and quality of care. Consider a scenario in which a PT and a PTA are not often in the same vicinity (home health, skilled nursing facility, or acute care). A plan of care that contains an adequate level of detail, in conjunction with the individual's anticipated goals, can ensure much better coordination of care. Written communication should provide the details of when the individual should be reevaluated by the PT before the plan of care is progressed.
In summary, providing increased detail in the initial goals and the treatment plan identifies the expected progression of the patient or client. The PT-PTA team can follow the individual's progression more closely and identify any unanticipated problems or red flags more readily. A detailed plan of care allows the PT to easily identify the individual's progression (or lack of progression).
Conclusion of Care Disposition Planning
It is good practice to anticipate the conclusion of care (discharge) planning from the start of every episode of care. This is particularly important in settings in which a physical therapist's evaluation assists in determining dispositions or transitions of care, or when the conclusion of care planning takes time and coordinated effort with other health care professionals. In other circumstances, a conclusion of the care disposition plan may be included in a prognosis statement. When a PTA has performed interventions under the PT's supervision, the PTA provides information for the PT to include in documentation, but the PT is solely responsible for writing the discharge notes.
Pediatric Patients and Clients
In certain pediatric settings, the conclusion of care may include additional factors. In early intervention and school-based practice, disposition planning is referred to as transition planning and will be documented in the pediatric patient's IFSP and IEP, respectively. The transition plan to conclude physical therapist services should be collaborative and based on the patient's needs. Individual students may not require skilled physical therapy every year they attend school. Skilled physical therapist services may be concluded in one year but referred again the next year as the patient's individual needs and physical environment change.
Outcomes
Outcomes are the actual results of implementing the plan of care that indicate the impact on functioning (body functions and structures, activities, and participation).
Per the "Guide to Physical Therapist Practice," as the individual reaches the end of the episode of care, the physical therapist measures the global outcomes of the services provided by characterizing or quantifying the impact of the physical therapist intervention on the following domains, based on suitability for and the circumstances of the patient or client:
- Pathology and pathophysiology (disease, disorder, or condition).
- Impairments in body function and structure.
- Activity limitations.
- Participation restrictions.
- Risk reduction and prevention.
- Health, wellness, and fitness.
- Societal resources.
- Patient or client satisfaction.
The physical therapist engages in outcomes data collection and analysis — that is, the methodical analysis of outcomes of care in relation to selected variables (e.g., age, sex, diagnosis, interventions performed) — and develops statistical reports for internal or external use.
The physical therapist also uses standardized outcome measures throughout the episode of care as part of periodic examinations that provide information regarding whether outcome expectations are being met. If expectations are not being met, the physical therapist determines whether or not to modify the plan of care and whether or not to reconsider the initial prognosis. The physical therapist also determines whether there is a need to refer to or consult with another practitioner.
Outcome Measurement at Conclusion of Episode of Care
Prior to concluding the episode of care, the physical therapist measures the individual's outcomes. Outcome measures are expected to identify changes in functioning; however, the physical therapist also considers changes to the environment to ensure that the change in functioning can be accurately attributed to the intervention. For example, a person may return to work not only because their functioning has changed but also because there may be monetary or family pressures or other personal or contextual factors that have an impact on outcomes.
Based on the results of the outcome measurement, the physical therapist determines the outcome status of the patient or client and whether the identified goals have been met. The physical therapist documents the individual's status and the rationale for the conclusion of care.
Physical therapists gather outcome measurements not only to determine the success of interventions within or at the end of an episode of care and to obtain information about the individual's perspective on progress, but also to contribute to comparative effectiveness research. The measurement data that physical therapists collect and analyze helps demonstrate the value and impact of physical therapist services on the health of society.