By using this site, you are consenting to our use of cookies. To find out more visit our privacy policy.
Some of the most exciting advances in physical therapist practice involve emerging digital technologies. Digital health — the integration of medical knowledge with technology to improve care and self-efficacy — has the potential to transform health care delivery with remote monitoring, health care apps, virtual reality, robotics and wearable sensors, augmented intelligence, and machine learning.
PTs and PTAs are increasingly using digital health technologies to expand and modify care delivery. In the right applications, these tools can advance quality of care, provide clinician support, speed access to services, increase patient engagement, and reduce overall spending.
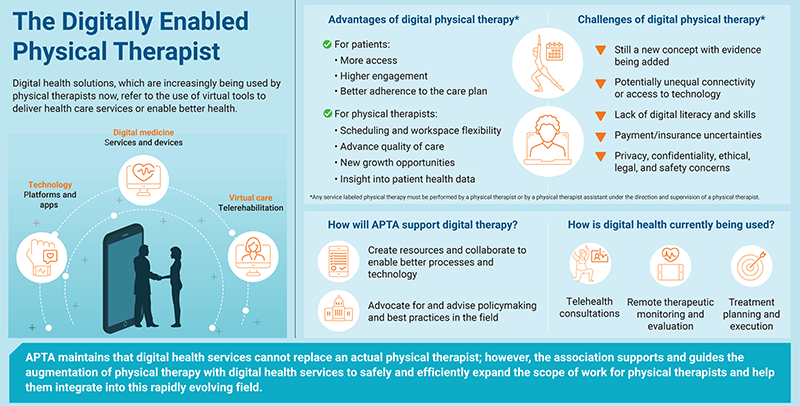
APTA has identified the concept of the digitally enabled physical therapist as a framework for addressing the role of digital health in physical therapy care. Digital technologies can never replace the value or role of the PT or PTA but can enable clinicians to expand their reach and deliver critical data on patient progress and outcomes.
APTA is dedicated to consumer transparency and is asking digital health providers for pledged commitments that digital physical therapy services only be performed or directed by licensed PTs, to be consistent with term and title protection efforts.
Before you begin practicing telehealth in your state:
- Examine your state's physical therapy licensure law and corresponding state licensure board regulations/rules. In many states, the physical therapy practice act is silent on the use of telehealth.
- You may wish to contact your state licensure board to ensure there are no limitations or restrictions for practicing telehealth.
- Check out APTA's Telehealth Certificate Series and Moving Forward with Telehealth in Physical Therapy to ensure that the physical therapy profession is prepared to provide excellent care via telehealth.
- Consideration for telehealth billing and coding can be found here, as well as resources on telehealth advocacy.
- This APTA CPG from 2024 provides 7 recommendations that address the impact of, preparation for, and implementation of telerehabilitation in physical therapist practice.
APTA and the Organization for the Review of Care and Health Apps, or ORCHA, have developed a collection of digital health apps and other products for the physical therapy profession that ORCHA has independently and objectively assessed for safety and effectiveness. The APTA Digital Health App Library, powered by ORCHA, is exclusive to association members and gives you a single source for choosing among quality-assured digital health tools to use and recommend to your patients and clients. Learn more.
Recommended Content
Aug 1, 2023 / Feature
With digital health use and cyberattacks both on the rise, here’s what physical therapy practices can do to ensure privacy and security.
Mar 13, 2023 / Roundup
We've updated an APTA practice resource, advocated for continued patient access, and alerted MACs to denials they're making in error.
Dec 22, 2020 / Article
Using telehealth to deliver physical therapist services is expanding rapidly, and if you haven't already, you're probably considering it.
Nov 21, 2022 / Resource
This foundational paper is intended to provide APTA members with information on the current landscape of digital health in physical therapy.
Aug 1, 2022 / Column
While technology shows promise for cutting-edge treatment, PTs and PTAs must ask the right questions to determine the best plan of care.
Additional Digital Health in Practice Content
May 24, 2023 / News
The decision to back off from locally based coverage decisions was fueled by APTA advocacy efforts.
Apr 14, 2023 / News
APTA's outreach sparked the change, to be made official in July. Until then, denied claims should be resubmitted.
Jun 21, 2022 / Review
Researchers say the CMS telehealth waivers worked and should be made permanent.
Apr 10, 2023 / Review
Authors of an article in PTJ say that telehealth-only and hybrid approaches were on a par with a six- to seven-session clinic-based program.
Jan 29, 2026 / Resource
The Medicare Physician Fee Schedule final rule for 2022 added five CPT codes for remote therapeutic monitoring. Physical therapists may bill these RTM codes under Medicare, and the codes also may be billable under commercial insurance plans. The new codes are available in the Medicine Section of the CPT Manual.
Jan 23, 2023 / News
APTA advised private practice PTs to continue direct supervision for PTA use of remote therapeutic monitoring until CMS clarified the issue.
Nov 22, 2022 / News
A new foundational paper provides context and considerations as more entities sign on to APTA's transparency pledge.
Sep 19, 2022 / Review
A systematic review involving more than 200,000 patients with a variety of conditions revealed consistently positive results for telerehab.
Jun 10, 2022 / Review
A program provided entirely via real-time video achieved outcomes comparable to in-person treatment, researchers say.
Sep 20, 2022 / Article
As digital health technology continues to evolve and incorporate into clinical care, APTA has identified resources from the international community that can enhance your digital literacy.